This year the International Stereotactic Radiosurgery Society (ISRS) 2024 was hosted in New York City. More than 340 abstracts were accepted, and over 630 attendees representing 53 countries and specialties including neurosurgeons, radiation oncologists, physicists, and more took part to learn, share, and excel!
We met up with Prof. Marc Levivier former President of ISRS and Arjun Sahgal, new President of ISRS to get their insights on the purpose of ISRS, benefits to members, ISRS certifications and what the future holds. Insert videos here.
Highlighting Abstracts for Brain Cancer Awareness Month
Safety and efficacy of CyberKnife radiosurgery for limited number of large volume brain metastases: analysis of single center real-world data1
This study aimed to assess the effectiveness of hyperfractionated radiosurgery on the CyberKnife® System as a treatment approach for a limited number (<3) of large-volume brain metastases patients. A prescribed dose of 21-34 Gy was delivered in 3-5 fractions using the CyberKnife System. The primary objective was to identify the overall survival after salvage treatment. Forty patients were included in the study. The one-year overall survival rate following fractionated SRS (FSRS) was 75%. Positive imaging responses were observed in 90% of the cohort and a significant clinical improvement was seen, as evidenced by the best Karnofsky performance scale score. Toxicity remained low with 12 patients experiencing grade 1 or 2 fatigue, and 4 patients reported Grade 3 headache. Additionally, progression-free survival for brain metastases from non-small-cell lung cancer (NSCLC) was significantly longer compared to other cancer types. FSRS with the CyberKnife System showed favorable clinical and radiologic control for limited number large volume brain metastases. An ongoing multicenter prospective observational study is being conducted to assess the efficacy of FSRS for limited brain metastases from NSCLC.
Safety and efficacy of CyberKnife radiosurgery plus anlotinib hydrochloride in patients with recurrent glioblastoma: a prospective phase II single-arm study2
Glioblastoma (GBM) is a highly vascular tumor with limited treatment options, especially upon disease recurrence. Targeted therapies such as bevacizumab aim to slow the growth of new blood vessels and is an established drug for treating recurrent glioblastoma (rGBM). A different targeted therapy drug called anlotinib is a multi-target tyrosine kinase inhibitor that can directly target the vascular endothelial growth factor receptor, platelet-derived growth factor receptor, and fibroblast growth factor receptor. In this study it was proposed that the anti-angiogenic effect of anlotinib may exceed that of bevacizumab, indicating promising treatment potential. This prospective phase II study reported the treatment effectiveness of combining anlotinib with SRS using the CyberKnife System treating 22 patients with rGBM. Patients who underwent surgery, standard radiotherapy, and temozolomide who were diagnosed with recurrence were selected for treatment. Each patient underwent SRS with 25Gy in 5 fractions in combination with oral administration of anlotinib (12 mg, daily, days 1–14/3 weeks). The primary objective was median overall survival (OS). Twenty-one patients exhibited tumor response, with 6 achieving complete response, resulting in an objective response rate of 95.5%. Median overall survival was 19.5 months. The combination of salvage SRS with anlotinib demonstrated promising outcomes and manageable toxicity in managing recurrent GBM.
10-year outcome after central dose optimized robotic stereotactic radiotherapy for brain metastases from different histologies3
SRS and FSRS have become the standard of care for limited brain metastases over the last decade. This study evaluated SRS and FSRS with the CyberKnife System over the past 10 years. Three hundred and twenty-three patients of different histologies with a total of 1164 brain metastases (BM) were treated. Targeted therapies and/or immunotherapy were given in 25.1% of cases. The number of brain metastases ranged from 1, 2-10 and >10 in 110, 195 and 18 cases, respectively. Eighty-one had received whole brain radiotherapy (WBRT) before SRS/FSRT. The mean follow-up period was 14.8 months and the median OS was 8.7 months. The most significant prognostic factor for longer OS was Karnofsky performance status of ≥90%. Overall PTV <2.6ccm was also associated with a longer OS of 15 months vs. 10 months with overall PTV ≥2.6ccm. Application of targeted therapy led to prolonged OS of 14.5 vs. 10.6 months. Local control after 12 months was 92.4%. The conclusion found that SRS and FSRT with the CyberKnife System is effective.
CyberKnife stereotactic radiosurgery for vestibular schwannoma: meta-analysis of long-term tumor control and hearing preservation outcomes4
This study reviewed literature describing outcomes of radiosurgery using the CyberKnife System for vestibular schwannoma, with particular focus on tumor control, hearing preservation, and dosing schema. Fifteen studies were included in the final analysis comprising 2,018 treated patients, of whom 64 had neurofibromatosis type 2 and the remaining had sporadic lesions. Three hundred nine patients had undergone prior treatment – surgical resection and/or radiosurgery and mean follow-up for the entire cohort was 40.0 months. Fractions ranged from 1-5 and isodose lines were reported in 13/15 studies and ranged from 55%-95%. The average local control across all studies was 96.0%. For patients with serviceable hearing pre-treatment, 73% had preserved hearing at the last follow-up. This meta-analysis demonstrated that SRS with the CyberKnife System offers high rates of local control and hearing preservation in patients undergoing SRS for vestibular schwannomas.
CyberKnife Stereotactic Radiosurgery for Extramedullary Plasmacytoma in the External Auditory Canal: A Clinical Case Report5
A case report of a 72-year-old man with a history of multiple myeloma, presenting with recurrent left external auditory canal plasmacytoma. The patient received initial conventional radiotherapy then developed a recurrence seven years later. The patient underwent stereotactic radiosurgery with the CyberKnife System, leading to complete resolution of the lesion without any long-term adverse effects or irradiation-related complications over a 45-month period. The case report highlights SRS as an effective approach in managing complex plasmacytomas.
Thought-Provoking Sessions at ISRS
AI in radiosurgery
At an ISRS session attendees learned about the current and potential applications of artificial general intelligence (AGI) in medicine and radiation oncology. AGI’s ability to process multimodal clinical data spanning visuals and text enables support at every stage from consultation to follow-up.
However, realizing AGI’s potential requires seamless integration with existing medical systems. A key limitation is AGI’s dependence on domain-specific knowledge, which can be addressed by incorporating comprehensive clinical datasets and interdisciplinary collaboration.
While current large language models (LLMs) and vision models are trained on general web data, fine-tuning them with high-quality medical data holds promise. Challenges include data standardization, sharing individual patient data due to privacy concerns, and interpretation of complex clinical data.
User-centered design involving interdisciplinary teams with radiation oncologists and medical physicists is crucial for clinical usability. While challenges remain regarding datasets, regulation, and collaboration, the opportunities for AGI to advance radiotherapy automation and improve clinical outcomes are significant.
The key takeaway was that introducing AGI has the potential to revolutionize radiation oncology by enhancing safety, precision, efficiency, and patient outcomes throughout the radiotherapy workflow. But it does not replace health care professionals, it should be used as an aid and not as an alternative to the medical profession. This is a rapidly evolving field, stimulating advancements and discussions for the benefit of healthcare.
Access disparities
Another session explored the disparities in access to SRS and stereotactic body radiotherapy (SBRT) across regions. One study delved into the variability of prescribing practices for central nervous system (CNS) metastases in Latin America and Spain.
The researchers conducted a survey among 106 SRS specialists, with 93.4% of participants from Latin America and 6.6% from Spain. The respondents included 87% radiation oncologists and 13% neurosurgeons, utilizing various technologies. The survey focused on specific questions regarding SRS dosing for CNS metastases of breast and renal cancers, particularly in the context of single-fraction SRS practice.
The findings revealed a striking variability in dose prescription for the same histological types, highlighting the need for a consensus in SRS practice for CNS metastases, at least within the Latin American region. The results underscored the importance of establishing international guidelines for standardization in SRS dosing for single-fraction CNS metastases.
By achieving uniformity in prescription practices, more homogeneous comparisons between studies and technologies can be facilitated, ultimately leading to more robust and reliable results. This presentation shed light on the critical need for consistent guidelines to ensure equitable access and optimal treatment outcomes across diverse geographical regions.
Learn more about ISRS and the benefits of being a member with Birgit Fleurent, ISRS Strategy Leader
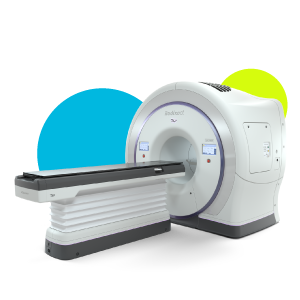
Learn more about the CyberKnife System
References
- E39Safety and efficacy of cyberknife radiosurgery for limited number of large volume brain metastases: analysis of single center real-world data. Yun GUAN (Shanghai, China), Wei ZOU, Li PAN, Enmin WANG, Yang WANG, Xin WANG
- 39602 OR053 Safety and efficacy of cyberknife radiosurgery plus anlotinib hydrochloride in patients with recurrent glioblastoma: a prospective phase II single-arm study (HSCK-002). Yun GUAN(Shanghai, China), Wei ZOU, Li PAN, Enmin WANG, Yang WANG, Xin WANG
- E6910-year outcome after central dose optimized robotic stereotactic radiotherapy for brain metastases from different histologies. Olaf WITTENSTEIN (Kiel, Germany), Fabienne DUY, Melanie GREHN, Robert WOLFF, Michael SYNOWITZ, Juergen DUNST, Hajrullah AHMETI, Oliver BLANCK, David KRUG
- E3CyberKnife stereotactic radiosurgery for vestibular schwannoma: meta-analysis of long-term tumor control and hearing preservation outcomes. Nolan BROWN (Los Angeles, USA), Zachary PENNINGTON, Brian LIEN, Redi RAHMANI, Julian GENDREAU, Josh CATAPANO, Michael LAWTON
- E229CyberKnife Stereotactic Radiosurgery for Extramedullary Plasmacytoma in the External Auditory Canal: A Clinical Case Report. Surya PATIL, Elaheh SHAGHAGHIAN, Lorenzo YUAN, Aaryan SHAH (Stanford, USA), Neelan MARIANAYAGAM, David PARK, Scott SOLTYS, Anand VEERAVAGU, Iris GIBBS, Gordon LI, Steven CHANG